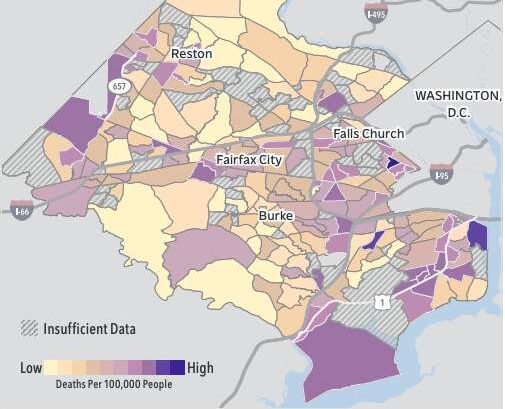
Black residents have experienced worse health outcomes than other populations across Northern Virginia, especially during the COVID-19 pandemic, a new report found.
Commissioned by the Northern Virginia Health Foundation (NVHF) and conducted by the Center on Society and Health at Virginia Commonwealth University, the Fairfax County section of the “Dying Too Soon” report found “stark” disparities across the county in the rates at which people die before the age of 75.
The report attributed the dramatic differences in life expectancies — from 76.5 years to 91.1 years — to an individual’s race, ethnicity and address, reflecting the influence of socioeconomic conditions on health outcomes.
According to the report, a lack of access to health care contributed to 66% of premature deaths in the county from 2015-2019 that were avoidable with preventative measures or treatment.
Throughout Northern Virginia, premature deaths are more concentrated within “islands of disadvantage,” where residents experience poor living conditions, higher mortality rates, and food and housing insecurity, the report says.
Residents of these neighborhoods are more likely to be people of color and immigrants, a disparity resulting from “the region’s history of segregation and systemic racism” and policies that “systematically block access” to health opportunities and increase exposure to unsafe health conditions, the report said.
Prior to the pandemic, Black people in Fairfax County had a premature death rate of 221.0 per 100,000 residents, exceeding the rates for white people (165.8 per 100,000), Hispanics (126.2 per 100,000) and Asians and Pacific Islanders (112.4 per 100,000).
Those disparities were consistent throughout the region, which “exhibits smaller racial-ethnic disparities” that other parts of the U.S., according to the report.
Though Fairfax County is often touted as one of the richest counties in the U.S., with a median income of $133,974, many of the wealthiest census tracts are located just a few blocks from islands of disadvantage.
In fact, the study says one census tract in Springfield has a premature death rate twice as high as that of a census tract in Franconia only two miles away. Each census tract also showed drastically different education and poverty rates and racial and ethnic compositions.
“I don’t think there’s a sense among the general public that these kinds of health inequities exist in a wealthy area like Northern Virginia, which in aggregate is doing quite well and has a very high quality of life,” Dr. Steven Woolf, lead study author and director emeritus of VCU’s Center on Society and Health, told FFXnow. “But when you zoom in like this to see what’s actually happening, neighborhood by neighborhood, you expose these these pockets of disadvantage that we want the public to know about.”
Census tracts with the highest premature death rates were in Seven Corners/Bailey’s Crossroads and Route 1 regions, according to the report’s summary. The study also reported that poverty rates in Seven Corners/Bailey’s Crossroads, Mount Vernon and Oakton “exceeded 20%, higher than poverty rates in countries like Estonia, Lithuania, Peru, Tajikistan, and Uganda.”
The Covid pandemic only worsened inequitable health outcomes, according to data collected in 2020-2021. The report says the county’s islands of disadvantage “experienced higher COVID-19 death rates,” and Northern Virginia as a whole saw “much higher” death rates among Hispanic and Black populations compared to Asian and white groups.
“COVID-19 simply pulled the veil back to show the public how bad these inequities are, but they’ve been with us for a very long time,” Woolf said. “There are policies of exclusion that limit the ability for people of color and low-income families to access opportunities and for health and wellbeing, and those barriers persist and will remain long after the COVID-19 pandemic has passed unless we change our policies.”
To combat these longstanding, widespread disparities, the study calls for increased access to health insurance and services, such as high-quality and affordable primary care, preventative care and chronic disease treatment. It further pushes for an increase in funding for “chronically underfunded” local public health departments that are still recovering from the “heightened demands” created by the pandemic.
The report also advocates for remedying “deficiencies” in the local behavioral health system by addressing shortages in mental health professionals and expanding access to mental health and substance abuse services.
Woolf emphasized the need to fund “social determinants of health,” including “education, jobs, fair wages, [and] affordable housing and transportation” to create more equitable outcomes.
“Data like ours that identify the precise census tracts experiencing the greatest threats to health and wellbeing can provide important insights to policymakers, service providers and funders,” NVHF President and CEO Patricia N. Mathews said in a press release. “They can help target investments in neighborhoods that have been neglected and prioritize efforts to improve living conditions by offering more affordable housing, expanding educational opportunities, and improving opportunities for employment.”
The report that NVHF released in 2017 identifying islands of disadvantage in the region has helped inform Fairfax County’s implementation of the One Fairfax policy, which commits local officials to considering equity when developing policies and services, says county Chief Equity Officer Karla Bruce.
“[The] most recent report, Dying Too Soon, illustrates the connection between social and economic conditions and health disparities and validates the value of the county’s investments in things like health care access, affordable housing, education, and workforce readiness,” Bruce said.
“The opportunity for good health should be available to all residents of Fairfax County,” the study concludes.


